Persistent Pulmonary Hypertension of the Newborn (PPHN)
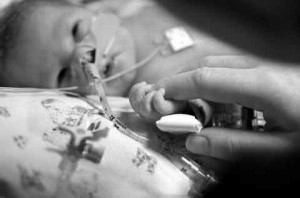 Selective serotonin reuptake inhibitors (SSRIs) are the most commonly prescribed antidepressants. They can ease symptoms of moderate to severe depression, but they can also increase the risk of severe birth defects. Clinical research has revealed that newborns are six times more likely to have persistent pulmonary hypertension, or PPHN, when their mothers take SSRIs (including Prozac, Paxil and Zoloft) during pregnancy.
Selective serotonin reuptake inhibitors (SSRIs) are the most commonly prescribed antidepressants. They can ease symptoms of moderate to severe depression, but they can also increase the risk of severe birth defects. Clinical research has revealed that newborns are six times more likely to have persistent pulmonary hypertension, or PPHN, when their mothers take SSRIs (including Prozac, Paxil and Zoloft) during pregnancy.
PPHN impacts the circulatory system of the infant and restricts oxygen flow to organs. Babies who survive this potentially fatal condition may suffer debilitating complications throughout their lives.
PPHN is a birth defect that damages the circulatory system. It occurs in roughly one newborn in every 500. With the condition, newborns are unable to breathe air normally after receiving oxygen in utero through the umbilical cord.
Oxygen is distributed through the body by the ductus arteriosus, a unique pulmonary artery. After birth when the umbilical cord is severed, the newborn normally starts breathing and the pulmonary blood pressure drops. The ductus arteriosus should narrow and then close. Blood flowing to the lungs normally goes up and oxygen is distributed around the body.
Infants with persistent pulmonary hypertension don’t undergo this normal series of events. The ductus arteriosus stays open and blood pressure in the lungs doesn’t go up. This strains the heart, which is working hard to deliver oxygen-rich blood throughout the lungs. More problems result as organs (such as the heart, lungs and brain) are injured because they’re not supplied enough oxygen.
Symptoms and complications associated with PPHN
Persistent pulmonary hypertension symptoms in newborns include:
- Cyanosis, evidenced by skin with a blue tinge
- Shortness of breath
- Hepatomegaly (enlarged liver)
- Heart murmur
- Edema in the hands or feet
- Insufficient blood-oxygen level
- Low blood pressure
- Rapid breathing
- Rapid heart beat
- Lethargy
- Excessive sweating
- Weak pulse
Long- lasting complications of PPHN may entail:
- Scarred, inflexible lungs
- Kidney failure
- Cerebral palsy
- Heart failure
- Problems with breathing
- Bleeding in the brain
- Seizures
- Deafness
- Injuries to internal organs
Diagnosis and treatment of PPHN
Doctors may suspect PPHN when:
- The mother used high doses of aspirin or indomethacin for a prolonged period during pregnancy
- The baby endured a stressful delivery
- The newborn has severe respiratory distress
- The newborn’s oxygen levels are unexpectedly low
A chest x-ray may be normal if there are no underlying lung problems. An echocardiogram to evaluate the pressure in the pulmonary arteries is required for a definitive diagnosis of PPHN.
Treatment involves placing the newborn in an environment with 100% oxygen. A ventilator may be needed in severe cases. A high percentage of oxygen in the blood helps open the arteries going to the lungs. In very severe cases, a very small amount of nitric oxide gas may be added to the oxygen. It opens the arteries in the newborn’s lungs and reduces pulmonary hypertension. This treatment may be needed for several days.
If all else fails, extracorporeal membrane oxygenation (ECMO) can be used. In this procedure, blood from the newborn is circulated through a machine that adds oxygen and removes carbon dioxide and returns the blood. ECMO has been lifesaving in cases where other treatments have failed, allowing some newborns with persistent pulmonary hypertension to survive until the condition resolves.
Persistent pulmonary hypertension of the newborn and SSRI’s
SSRI’s are some of the country’s best-selling and familiar pharmaceuticals. Drugs in this class include Zoloft (sertraline), Prozac (fluoxetine), Celexa (citalopram), Paxil (paroxetine), Symbyax (fluoxetine with atypical antipsychotic olanzapine) and Lexapro (escitalopram). They benefit many Americans but they are also associated with serious side effects. The FDA announced in 2005 that using Paxil (paroxetine) while in the first trimester of pregnancy might “increase the risk for congenital malformations, particularly cardiac malformations.” The agency asked Paxil’s manufacturer, Glaxo Smith Kline, to include new warnings concerning paroxetine use by pregnant women. Pexeva, Paxil, Paxil CR and paroxetine hydrochloride all contain paroxetine.
A February 2006 study in The New England Journal of Medicine linked SSRI use among pregnant patients to PPHN. The authors found PPHN was six times more likely to develop in newborns whose mothers used SSRI’s after the 20th week of pregnancy. In July 2006, the FDA published a public health advisory concerning the treatment of pregnant women with SSRI’s and the risk of heart problems like persistent pulmonary hypertension. The advisory stated the FDA was seeking more information about that risk and asked SSRI manufacturers to change the drugs’ warnings to include the possible risk of PPHN.
A drug safety communication was issued by the FDA in 2011 stating there were “conflicting findings” concerning a link between SSRI’s and PPHN. The FDA stated no solid conclusions could be determined.
Other birth defects have been linked to SSRI use by pregnant women. A 2010 study in the American Journal of Nursing determined that babies exposed to SSRI’s in the uterus have a greater chance of many complications, including heart defects. A Danish study published in 2009 showed the overall risk for congenital heart problems associated with SSRI use by pregnant women are low. However, babies born to women who had filled prescriptions for more than one SSRI had a four-fold increase in septal heart defects — a malformation of the wall that divides the left and right sides of the heart. Of the more than 400,000 children in the study, septal heart defects occurred in 0.5% of children born to mothers who did not take antidepressants and 0.9% of children born to mothers who did.
- WebMD, Antidepressants Linked to Birth Defect, http://www.webmd.com/baby/news/20090924/antidepressants-linked-to-birth-defect
- National Institute of Health, Persistent pulmonary hypertension of the newborn , http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3740154/
- Merck Manual, Persistent pulmonary hypertension, http://www.merckmanuals.com/home/childrens_health_issues/problems_in_newborns/

 Resources
Resources
 Resources
Resources